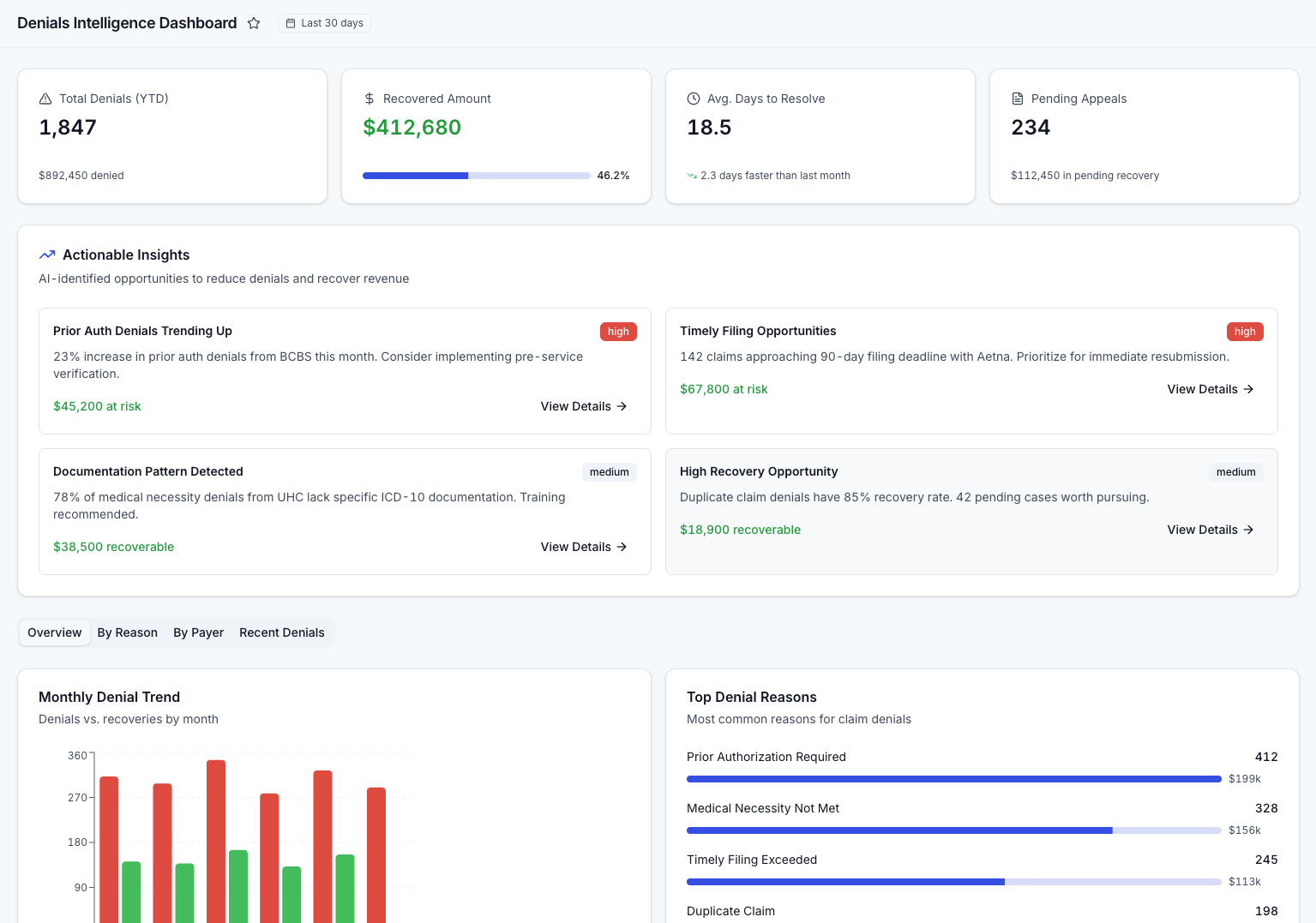
Denials Intelligence
AI-powered denial pattern recognition with root cause analysis.
Everything you need
Data Integration
Connect EMRs, billing, labs, and scheduling. We normalize and validate across all sources.
Unify AthenaHealth + clearinghouse data for complete claims visibility.
Live Dashboards
Real-time visualizations built for action. Custom views per role.
CFO sees revenue trends; billing sees denial patterns — same data, different views.
Automated Alerts
Threshold-based triggers that notify your team the moment something needs attention.
Alert when denial rate exceeds 8% for any payer in a rolling 30-day window.
Predictive Analytics
Forecast collections, patient volume, and staffing needs before they become problems.
Predict next month's cash flow based on current AR aging and historical patterns.
Workflow Automation
Trigger outreach, escalations, and follow-ups automatically based on your rules.
Auto-queue balance letters for accounts >90 days with no activity.
Export & Reporting
One-click exports, scheduled reports, and custom report builder.
Weekly board report auto-generated and emailed every Monday morning.
Not a BI tool. A healthcare intelligence partner.

See Unify Insights in action
Schedule a personalized demo and see exactly how we'd transform your data.